- Home
- Moving “Dual Eligibles” Into Mandatory M...
Moving “Dual Eligibles” Into Mandatory Managed Care and Capping Their Federal Funding Would Risk Significant Harm to Poor Seniors and People With Disabilities
As policymakers seek to reduce federal budget deficits, they may face proposals to reduce spending on low-income Medicare beneficiaries who also are eligible for Medicaid (the “dual eligibles”) by 1) requiring them to receive both their Medicare- and Medicaid-covered services through a single managed care plan that would operate under a contract with their state, and 2) imposing a cap on the funding their state would receive for that purpose. Such proposals would be ill-advised at this time.
Experts agree that we should try to find ways to better coordinate care for these beneficiaries that would improve quality of care while producing savings. But, we do not yet know how to do this. An array of demonstration projects designed to address this is about to begin across the country. Some past efforts to change the way care is delivered for this population have resulted in harm to vulnerable low-income beneficiaries, and careful testing to find what works safely and what doesn’t is in order. Jumping the gun before any demonstration project results are in, and mandating the placement of these low-income individuals into managed care now, would pose significant risks to some of the most frail and vulnerable people in the country.
Policymakers should abide by the Hippocratic Oath here and “do no harm.” We need to learn how best to coordinate care for this population, and what the respective roles of Medicare and Medicaid and the financial arrangements across the programs should be, before we make wholesale changes in federal policy. We may well find that a “one size fits all” approach — such as mandating the movement of most or all dual eligible beneficiaries into capitated (per-beneficiary) managed care arrangements — would be misguided and that differentapproaches to care coordination are needed for different groups within the dual-eligible population. Indeed, the Medicare Payment Advisory Commission (MedPAC), Congress’ expert advisory body on Medicare payment policy, has warned that “Given the diversity of the care needs of the dual-eligible population, a common approach to full integration and care coordination may not be best suited for all beneficiaries.”
Background on the Dual Eligibles
The approximately 9 million low-income elderly and disabled individuals who are the dual eligibles are poorer and sicker than Medicare and Medicaid beneficiaries as a whole, and consequently account for disproportionate shares of Medicaid and Medicare spending. Dual eligibles make up 15 percent of Medicaid beneficiaries but account for 39 percent of Medicaid spending; they make up 21 percent of Medicare beneficiaries but account for 36 percent of Medicare spending.[1]
Coordination across the two programs is lacking. According to a recent MedPAC report, “conflicting program incentives encourage providers to avoid costs rather than coordinate care,” which often results in high spending and low quality.[2] For example, Medicaid pays for most nursing home care and long-term care services while Medicare covers hospital stays and other acute care services, so efforts to improve care in nursing homes and avoid unnecessary hospitalizations glean savings for Medicare but not for Medicaid. That does not provide incentives for state Medicaid programs to make such improvements.
Given the widespread agreement on the need to improve the coordination and efficiency of care for dual eligibles, some policymakers may be tempted to act now to mandate major changes in how care is delivered to this population, in order to try to secure federal savings for deficit reduction. For example, the Bowles-Simpson commission report recommended giving states full responsibility for all health care services (both under Medicare and Medicaid) for dual eligibles and enrolling all dual eligibles in state-run managed care plans.
But although some new approaches to improving coordination of care for dual eligibles have shown significant promise, none have yet been proven to improve coordination of care and save money. That is why, subsequent to the issuance of the Bowles-Simpson report, the Congressional Budget Office (CBO) advised that requiring all dual eligibles to enroll in managed care would not itself produce any federal budgetary savings as the Bowles-Simpson report had assumed. The only way to achieve scoreable savings would be to move dual eligibles to managed care and impose an arbitrary cap on the amount of federal Medicare and/or Medicaid spending for the dual eligibles, with the cap set at a level below what the federal government would otherwise provide under current law.
Limiting or capping federal funding in this manner on a per-beneficiary basis would pose significant risks for low-income seniors and people with disabilities.[3] If states were unable to achieve substantial savings through managed care without impairing access to needed care, then — to make up for the reductions in federal funding and fit within the cap — they would either have to contribute significantly more of their own funding (an unlikely development) or scale back acute and long-term care services for dual eligibles.
A major series of state-based demonstration projects is about to begin to test various approaches to integrating and better coordinating care for the dual eligibles across Medicare and Medicaid. About half of the states will operate the demonstrations, with the first group scheduled to begin in 2013. Given the extensive and diverse health care needs of the dual-eligible population and the lack of proven approaches to successfully coordinate care across Medicare and Medicaid on a large scale, federal policymakers should await the results of these demonstrations rather than act precipitously to take risky steps such as moving large numbers of dual eligibles into managed care on a mandatory basis and capping federal funding for their health care services.
Dual Eligibles Are a Diverse Group With Varying Needs
To date, only a small number of programs with very limited numbers of participants have successfully coordinated Medicare and Medicaid services for dual eligibles. According to MedPAC, only 20 health plans have experience receiving capitated payments to provide dual eligibles with both Medicare and Medicaid services.[4] In part, this is because dual eligibles are diverse, so no one model of delivering care is likely to meet their varying needs for health care services.
Dual eligibles vary on a number of dimensions. About 6.8 million are “full dual eligibles” who receive hospital care, physicians’ services, prescription drugs, and other acute care services through Medicare and long-term care and other services that Medicare does not cover through Medicaid. The remaining dual eligibles, often called “partial duals,” receive all of their health care services through Medicare providers; Medicaid’s role is limited to helping cover their Medicare premiums and/or cost-sharing charges. Moving the partial duals to Medicaid managed care plans would likely force many of them to change health care providers.
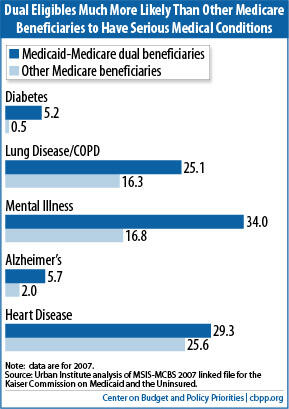
Adding to these concerns is the fact that many dual eligibles have multiple chronic conditions.[5] As noted, they are sicker and more vulnerable than other Medicare beneficiaries, on average.[6] They also are much poorer.
- Over half have incomes less than $10,000 a year, compared to 8.3 percent of Medicare beneficiaries who are not dual eligibles.[7]
- They are more likely to be eligible for Medicare because of a serious disability: some 38 percent of dual eligibles are people under 65 with serious disabilities, compared to 12 percent of other Medicare beneficiaries.
- They also are more likely to have a mental illness — 34 percent do, compared to 16.8 percent for other Medicare beneficiaries — or a cognitive impairment. For example, 5.7 percent of dual eligibles have Alzheimer’s, compared to 2 percent of other Medicare beneficiaries.[8]
While care for dual eligibles is more costly overall than care for other Medicare and Medicaid beneficiaries, there is little overlap between the dual eligibles with high Medicare spending and those with high Medicaid spending. This is largely because of the division of responsibility between Medicaid and Medicare: costs for dual eligibles with high Medicaid spending primarily reflect long-term care, while costs for dual eligibles with high Medicare spending mostly reflect acute care.[9] This means that interventions to improve care and lower costs for beneficiaries with high health care costs will differ depending on whether they target people with high costs in Medicare, Medicaid, or both.[10]
Capping funding for health care services at a rate below what would otherwise be spent — based on the expectation that such initiatives will generate savings, even though the evidence to date has shown otherwise— would compound the difficulties that beneficiaries could face. These difficulties would worsen if health care costs subsequently grew faster than had been anticipated for justifiable reasons, such as breakthroughs in treating heart disease, various cancers, Parkinson’s, Alzheimers’, diabetes, or the like that markedly improve health but add to costs. If the capped funding amounts did not rise in response to these increases, dual eligibles could be denied vital treatments.
Capping Funding for Dual Eligibles Would Likely Reduce Access to Needed Care
Proposals to cap funding for dual eligibles differ somewhat from proposals that some policymakers have made to impose per capita caps on the entire Medicaid program, since they would apply to both Medicaid and Medicare funding combined (and only to care for dual eligibles). Nevertheless, they raise a number of similar issues.
- To produce federal budgetary savings, the combined Medicaid and Medicare caps would have to be set at a level below what the federal government would provide under current law. This would likely be accomplished by adjusting the per-beneficiary cap amounts each year by a factor that grows more slowly than the growth rate currently projected for Medicare and Medicaid spending on dual eligibles, which reflects expected increases in health care costs.
- Because funding would grow more slowly than health care costs, funding shortfalls would likely emerge that would grow steadily larger over time. The shortfalls would be even greater if cost growth for dual eligibles turned out to be higher than had been anticipated because of the development of new treatments and medications or new medical technology, as noted.
- In addition, as the baby-boom generation (those born between 1946 and 1964) grows older, a larger share of seniors who are dual eligibles will become “old-old,” making them considerably more likely than “young-old” dual eligibles to be frail, have major health problems, and need long-term care services and supports. Because the annual adjustment to the funding caps would not (under proposals developed to date) account for these demographic shifts, the Medicaid and Medicare funding shortfalls would likely grow over time, particularly in states that experience larger-than-average increases in the number of dual eligibles who are older and have more serious infirmities.
- States would thus be under growing financial pressure to identify approaches to coordinating care for the dual eligibles that substantially lower costs. If the care coordination itself did not produce those results, states would have to make up for the funding shortfalls through increasingly large reductions in the services provided to dual eligibles, unless states contributed more of their own funds to fill the gap. (States would be unlikely to fully fill such a gap because it would include the costs of health services that previously were fully federally funded under Medicare.) Given that many dual eligibles rely on long-term care services and supports, this could mean significant cuts to nursing home care and in-home services, among other reductions in health care services.
- People with disabilities who rely on services like personal care attendants to allow them to live and work in the community would likely be at special risk if states found it difficult to eliminate or sharply cut services for people in nursing homes and other institutional settings.
No Proven Approaches Yet to Improving Care While Lowering Costs
Only a very small percentage of dual eligibles are now in programs that coordinate some or all Medicaid and Medicare services.[11] A few such programs, such as the Program of All-Inclusive Care for the Elderly (PACE), have successfully integrated Medicaid and Medicare services and raised the quality of care provided to dual eligibles. (PACE providers receive payments from Medicare and Medicaid and blend those funds to cover health care and other services for program participants.) But fewer than 1 percent of dual eligibles are enrolled in PACE programs. And program costs have actually been higher under PACE than the projected Medicare and Medicaid fee-for-service costs for the same beneficiaries’ care.[12] Enrollment in other integrated programs, such as the Massachusetts Senior Care Options program, similarly is very small.
- Some dual eligibles are enrolled in “dual eligible special needs plans” (D-SNPs), which are Medicare Advantage plans that seek to improve care coordination for dual eligibles by offering all Medicare services through a single plan. But while some D-SNPs have a contract with their state Medicaid agency to manage Medicaid services, as well, most do not, and thus don’t coordinate care across both programs.[13] A study of D-SNPs concluded that “coordination between the Medicare and Medicaid programs is more a goal than a reality.”[14] In addition, there has been little evaluation of the performance of these plans in lowering costs and improving enrollees’ health outcomes,[15] and D-SNPs are concentrated in just a small number of states.[16]
- States also have had limited experience with Medicaid managed care for seniors and people with disabilities. In fiscal year 2008, only 2.2 percent of the enrollees in Medicaid managed care plans were seniors and only 10 percent were people with disabilities. As with Medicare, enrollment in Medicaid managed care plans that do cover seniors and people with disabilities is concentrated in a small number of states.
Given the sparse state experience with such approaches — and the limited success to date in lowering costs and increasing health-care quality — policymakers need to be cautious. A wholesale transfer of millions of dual eligible beneficiaries to managed care at this time would pose very substantial risks for seniors and people with disabilities. An arbitrary cap on federal funds below the levels that would otherwise be spent on these beneficiaries’ care would compound these risks.
Approaches to Integrating Care Should Be Tested Before Being Widely Adopted
The Affordable Care Act created the Federal Coordinated Health Care Office, now called the Medicare-Medicaid Coordination Office, to better integrate and more effectively coordinate care for dual eligibles.[18] This office has launched a series of demonstration projects scheduled to start in 2013 to test new models of service delivery and payment.
Federal officials expect about 20 states to participate in a three-year demonstration project that will provide a single capitated payment to health plans that provide both Medicaid and Medicare services to defined groups of dual eligibles within each state. Six additional states will participate in the demonstration project using a managed fee-for-service model. [19]
The demonstration projects are intended to better align financial incentives across Medicare and Medicaid by allowing states to share in Medicare savings from avoiding unnecessary hospitalizations and providing better coordinated care. The demonstrations are also intended to make participation in integrated care programs more attractive for health care plans by allowing states to use “passive enrollment” of Medicare beneficiaries, which is expected to increase enrollment. Under “passive enrollment,” beneficiaries are enrolled in managed care unless they affirmatively opt out.
The specific state plans for these demonstrations are still in the review stage. MedPAC has raised substantial concerns that some states are inappropriately including all or most dual eligibles in their demonstration projects and may be proceeding too quickly without paying sufficient heed to the diverse nature of the dual eligible population and the question of whether of managed care plans in the state are able to provide the needed care for this population. In a letter to HHS in July, MedPAC stated that the scope of the planned demonstrations is too broad, given health plans’ limited experience and capacity to manage the full range of Medicare and Medicaid services.[20]
Part of the concern is that dual eligibles could be assigned to managed care plans with networks that do not include their longstanding health care providers or could be enrolled in care coordination models not appropriate for their particular health and long-term care needs. It will be difficult for many dual eligibles, especially those with cognitive impairments, to make informed choices, so methods for informing beneficiaries and their families about their choices under the new arrangements will need to be developed carefully and tested.
Conclusion
MedPAC and others have raised concerns regarding the scope and speed of the health reform demonstration projects that are about to start. The hope is that these concerns will be appropriately addressed and the demonstration projects will produce results that can be applied on a larger scale to improve health-care quality while lowering costs. This, however, will take some time. Taking a shortcut by acting now to require that dual eligibles be enrolled in untested managed care plans — and to cap the federal funds available for these beneficiaries’ care at amounts below what would otherwise be expended — would pose significant dangers for large numbers of vulnerable low-income seniors and people with disabilities.
End Notes
[1] Kaiser Commission on Medicaid and the Uninsured, “The Diversity of Dual Eligible Beneficiaries: An Examination of Services and Spending for People Eligible for Both Medicaid and Medicare,” April 2012.
[2] MedPAC, “Report to the Congress: Aligning Incentives in Medicare,” June 2010.
[3] For a discussion of the risks of a per capita cap, see Edwin Park and Matt Broaddus, “Medicaid Per Capita Cap Would Shift Costs to States and Place Low-Income Beneficiaries at Risk,” Center on Budget and Policy Priorities, October 4, 2012.
[4] MedPAC, “Report to the Congress, Medicare and the Health Care Delivery System,” June 2012.
[5] Gretchen Jacobson, Tricia Neuman, and Anthony Damico, “Medicare’s Role for Dual Eligible Beneficiaries,” Kaiser Family Foundation, April 2012.
[6] Teresa A. Coughlin, Timothy A. Waidmann, and Lokendra Phadera, “Among Dual Eligibles, Identifying the Highest-Cost Individuals Could Help in Crafting More Targeted and Effective Responses,” Health Affairs, May 2012.
[7] The data in these bullets reflect all dual eligibles — i.e., both full and partial dual eligibles.
[8] Kaiser Commission on Medicaid and the Uninsured, supra, fn. 1.
[9] Jacobson, et al., supra, fn 5.
[10] Coughlin, et al. supra, fn. 6.
[11] MedPAC, “Report to the Congress: Medicare and the Health Care Delivery System,” June 2011.
[12] David C. Grabowski, “Special Needs Plans and the Coordination of Benefits and Services for Dual Eligibles,” Health Affairs, January/February 2009.
[13] By 2013, D-SNPs must have contracts with states. However, there is no requirement that the states actually contract with the D-SNPs, so there is no guarantee all D-SNPs will be able to fulfill the new requirement.
[14] Marsha Gold, Gretchen Jacobson, Anthony Damico, and Tricia Neuman, “Special Needs Plans: Availability and Enrollment,” Kaiser Family Foundation, September 2011.
[15] Grabowski, supra, fn. 12. James Verdier, Marsha Gold, Sarah Davis, “Do We Know if Medicare Advantage Special Needs Plans are Special?” Kaiser Family Foundation, January 2008.
[16] James M. Verdier, Melanie Au, Jessica Gillooly, “Managing the Care of Dual Eligible Beneficiaries: A Review of Selected State Programs and Special Needs Plans,” MedPac, June 2011.
[17] Medicaid and CHIP Payment and Access Commission, “Report to the Congress: “The Evolution of Managed Care in Medicaid,” June 2011. Comprehensive risk-based managed care plans are paid a fixed amount per member per month to cover all or most Medicaid-covered services.
[18] Section 2602 of the Affordable Care Act.
[19] Integrated Care Resource Center at http://www.integratedcareresourcecenter.com/
[20] MedPAC Letter to Marilyn Tavenner, July 11, 2012.
More from the Authors
