- Home
- Like Other ACA Repeal Bills, Cassidy-Gra...
Like Other ACA Repeal Bills, Cassidy-Graham Plan Would Add Millions to Uninsured, Destabilize Individual Market
In releasing a revised version of their legislation to repeal and replace the Affordable Care Act (ACA), Senators Bill Cassidy and Lindsey Graham, along with co-sponsors Dean Heller and Ron Johnson, claimed that their bill isn’t a “partisan” approach and doesn’t include “draconian cuts.” In reality, however, the Cassidy-Graham bill would have the same harmful consequences as those prior bills. It would cause many millions of people to lose coverage, radically restructure and deeply cut Medicaid, and increase out-of-pocket costs for individual market consumers. It would cause many millions of people to lose coverage, radically restructure and deeply cut Medicaid, eliminate or weaken protections for people with pre-existing conditions, and increase out-of-pocket costs for individual market consumers.
Cassidy-Graham would:
- Eliminate the ACA’s marketplace subsidies and enhanced matching rate for the Medicaid expansion and replace them with an inadequate block grant. Block grant funding would be well below current law federal funding for coverage, would not adjust based on need, would disappear altogether after 2026, and could be spent on virtually any health care purpose, with no requirement to offer low- and moderate-income people coverage or financial assistance.
- Convert Medicaid’s current federal-state financial partnership to a per capita cap, which would cap and cut federal Medicaid per-beneficiary funding for seniors, people with disabilities, and families with children.
- Eliminate or weaken protections for people with pre-existing conditions by allowing states to waive the ACA’s prohibition against charging higher premiums based on health status and the requirement that insurers cover essential health benefits including mental health, substance abuse treatment, and maternity care.
- Destabilize the individual insurance market in the short run — by eliminating the ACA’s federal subsidies to purchase individual market coverage and eliminating the ACA’s individual mandate to have insurance or pay a penalty —and risk collapse of the individual market in the long run.
- Eventually result in larger coverage losses than under proposals to repeal ACA’s major coverage provisions without replacement. The Congressional Budget Office (CBO) has previously estimated that repeal-without-replace would cause 32 million people to lose coverage. The Cassidy-Graham bill would likely lead to greater numbers of uninsured after 2026, however, because it would not only entirely eliminate its block grant funding — effectively repealing the ACA’s major coverage expansions — but also make increasingly severe federal funding cuts to the rest of the Medicaid program (outside of the expansion) under its per capita cap.
By attempting to push this bill forward now, Senators Cassidy and Graham are reverting to a damaging, partisan approach to repealing the ACA that would reverse the historic coverage gains under health reform and end Medicaid as we know it — even as other members of Congress, with the help of governors and insurance commissioners of both parties, are making progress in crafting bipartisan legislation to strengthen the individual market.
Block Grant No Replacement for ACA Coverage Provisions
Cassidy-Graham cuts health coverage in two ways: first, by undoing the ACA’s major coverage expansions through a block grant, and second, by radically restructuring and cutting the entire Medicaid program. The bill would eliminate the ACA’s Medicaid expansion and marketplace subsidies starting in 2020, offering in their place only a smaller, temporary block grant that states could use for health coverage or any other health care purposes, with no guarantee of coverage or financial assistance for individuals.
According to the bill’s sponsors, this block grant would give states “flexibility,” allowing them to maintain the coverage available under the ACA if they wanted to do so while enabling other states to experiment with alternative approaches. But in reality, states wouldn’t be able to maintain their coverage gains under the ACA. Instead, Cassidy-Graham, like the earlier House and Senate repeal-and-replace bills, would cause many millions of people to lose coverage.
First and foremost, this is because the block grant funding would be insufficient to maintain coverage levels equivalent to the ACA. The block grant would provide $243 billion less between 2020 and 2026 than projected federal spending for the Medicaid expansion and marketplace subsidies under current law. In 2026, block grant funding would be at least $41 billion (17 percent) below projected levels under the ACA. These figures do not include the cuts resulting from the bill’s Medicaid per capita cap, discussed below, which would cut Medicaid funding outside of the ACA’s Medicaid expansion by an estimated $39 billion in 2026.
These estimates understate the actual cuts to federal funding for health coverage in another way as well. Under current law, federal funding for the Medicaid expansion and marketplace subsidies automatically adjusts to account for enrollment increases due to recessions or for higher costs due to public health emergencies, new breakthrough treatments, demographic changes, or other cost pressures. In contrast, the Cassidy-Graham block grant amounts would be fixed — they wouldn’t adjust for the higher costs states would face due to these factors. Faced with a recession, for example, states would have to either dramatically increase their own spending on health care or, as is far more likely, deny help to people losing their jobs and their health insurance.
Like the earlier version of the Cassidy-Graham plan, the revised plan would disproportionately harm certain states. The block grant would not only cut overall funding for the Medicaid expansion and marketplace subsidies but also, starting in 2021, redistribute the reduced federal funding across states, based on their share of low-income residents rather than their actual spending needs. In general, over time, the plan would punish states that have adopted the Medicaid expansion or been more successful at enrolling low- and moderate-income people in marketplace coverage under the ACA. It would impose less damaging cuts, or even raise funding initially, for states that have rejected the Medicaid expansion or enrolled few low-income residents in marketplace coverage. (These states would still see large cuts in the long run and during recessions or when faced with other anticipated increases in health care costs or need.)
In 2026, the 20 states facing the largest funding cuts in percentage terms would be Alaska, California, Connecticut, Delaware, the District of Columbia, Hawaii, Kentucky, Louisiana, Maryland, Massachusetts, Minnesota, Montana, New Hampshire, New Jersey, New York, North Dakota, Oregon, Rhode Island, Vermont, and Washington. These states’ block grant funding would be anywhere from 35 percent to nearly 60 percent below what they would receive in federal Medicaid expansion and/or marketplace subsidy funding under current law.
The Cassidy-Graham bill would lead to large coverage losses for another reason as well. Under current law, moderate-income consumers in the individual market are guaranteed tax credits to help them pay for meaningful coverage meeting certain standards, and low-income adults in expansion states are guaranteed the ability to enroll in Medicaid, which provides a comprehensive array of benefits and financial protection. Cassidy-Graham would eliminate these guarantees and allow states to spend their federal block grant on virtually any health care purpose, not just for health coverage.
Facing federal funding cuts and exposed to enormous risk, most if not all states would have to use the bill’s so-called “flexibility” to eliminate or cut coverage and financial assistance for low- and moderate-income people. In particular, many states would likely do one or more of the following: cap enrollment; offer very limited benefits; charge unaffordable premiums, deductibles, or copayments; redirect federal funding from providing coverage to other purposes, like reimbursing hospitals for uncompensated care; and limit assistance to fixed dollar amounts that put coverage out of reach for most low- and moderate-income people. As a result, many millions of people would lose coverage.
Block Grant Funding Would End After 2026
The bill’s block grant would not only be inadequate to replace the ACA’s major coverage expansions (the Medicaid expansion and the marketplace subsidies) but would disappear altogether after 2026. The bill’s sponsors have claimed that the rules that govern the budget reconciliation process, which allows the bill to pass the Senate with only 50 votes, necessitated that the proposed block grant be temporary. In reality, however, nothing in those rules prevents the bill from permanently funding its block grant. Furthermore, the expiration of the temporary block grant would create a funding cliff that Congress likely couldn’t afford to fill. Even if there were significant political support for extending the inadequate block grant in the future, budget rules would very likely require offsets for the hundreds of billions of dollars in increased federal spending needed for each additional year.
The result is that, beginning in 2027, Cassidy-Graham would be virtually identical to a repeal-without-replace bill — except for its additional Medicaid cuts through the per capita cap, described below. CBO estimated that the repeal-without-replace approach would ultimately leave 32 million more people uninsured. The Cassidy-Graham bill would presumably result in even deeper coverage losses than that in the second decade.
Like Prior Repeal Bills, Cassidy-Graham Imposes Damaging Cuts to Rest of Medicaid Outside of Expansion
Like prior House and Senate Republican repeal bills, the Graham-Cassidy bill would radically restructure and cut the rest of Medicaid, outside of the ACA’s Medicaid expansion. It would end the federal-state financial partnership under which the federal government pays a fixed percentage of a state’s Medicaid costs. It would instead impose a per capita cap, under which federal Medicaid funding would be capped at a set amount per beneficiary, irrespective of states’ actual costs, and would grow each year more slowly than the projected growth in state Medicaid costs per beneficiary.
The result would be deep cuts to federal Medicaid spending for seniors, people with disabilities, families with children, and other adults (apart from those affected by the bill’s elimination of the Medicaid expansion). Earlier CBO estimates suggest that Cassidy-Graham would cut the rest of Medicaid (outside the expansion) by $175 billion between 2020 and 2026, with the cuts reaching $39 billion by 2026 or 8 percent relative to current law.[1]
These cuts would grow in coming decades. That’s because starting in 2025, the bill would lower the annual adjustment of per capita cap amounts. For example, the cap on Medicaid spending for children and non-disabled, non-elderly adults would rise each year by the general inflation rate, which is about 2.5 percentage points lower than projected increases in per-beneficiary costs for those groups. As CBO has previously found with the Senate Republican leadership bill (the Better Care Reconciliation Act), this would drive deeper federal Medicaid spending cuts over the long run as the “gap [between Medicaid spending under current law and under the per capita cap] would continue to widen because of the compounding effect of the differences in spending growth rates” between the per capita cap and states’ actual Medicaid spending needs.[2]
The per capita cap would force states to make the same kinds of harsh choices in the rest of their Medicaid program that are imposed on them by the bill’s other funding cuts. States would have to raise taxes, cut other budget priorities like education, or make increasingly severe cuts to eligibility, benefits, and provider payments. For example, many states would likely cut home- and community-based services, which allow people needing long-term services and supports to remain in their homes rather than move to a nursing home; these and other benefits that are “optional” to states under federal law would be at greatest risk.
Moreover, the gap between federal funding under the per capita cap and states’ actual funding needs would grow even larger if Medicaid costs grow more quickly than expected (due to a public health emergency or a new drug) or grow in ways that the per capita cap doesn’t account for (due to the aging of the population).
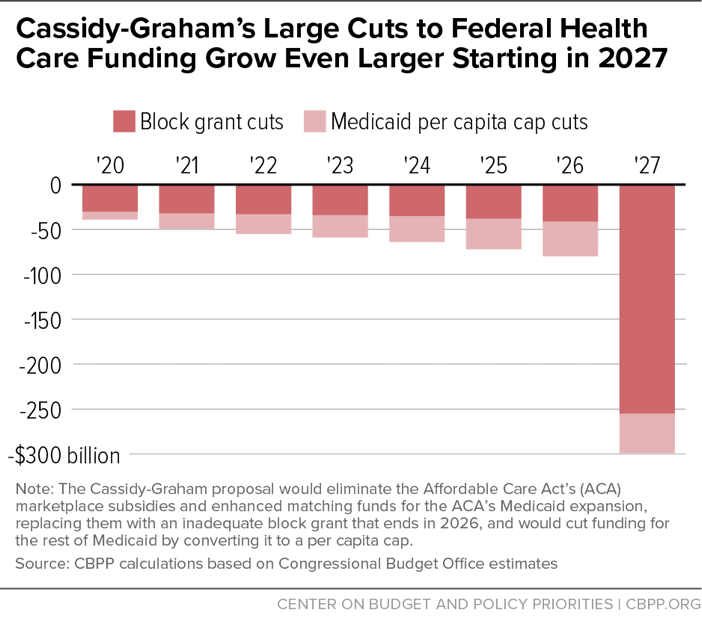
Notably, these per capita cap cuts would come on top of the cuts to Medicaid expansion funding and marketplace subsidies under the block grant discussed above. In 2026, for example, we estimate that the block grant and Medicaid per capita cap combined would result in at least a $80 billion federal funding cut. (See Figure 1.) Thirty-six states, including the District of Columbia, would face net cuts to Medicaid funding (not just for the expansion) and marketplace subsidies in that year. (See Appendix Table 1.) In 2027, when the block grant is eliminated entirely and the per capita cap cuts continue to grow, we estimate the combined federal funding cut would be $299 billion, relative to current law.[3]
Plan Would Eliminate or Weaken Pre-Existing Condition Protections
Similar to the House-passed bill (the American Health Care Act), the Cassidy-Graham bill would provide states expansive waiver authority to eliminate or weaken the prohibition against insurance companies charging higher premiums based on their health status and the requirement that insurers cover the essential health benefits related to any health insurance plan that is in any way subsidized by the bill’s block grant funding. States seeking waivers would only have to explain how they intend to maintain access to coverage for people with pre-existing conditions, but they wouldn’t have to prove that their waivers would actually do so.[4]
The block grant subsidy requirement, for example, could be satisfied by states simply using a small portion of their block grant funding to provide even tiny subsidies to all individual market plans. As a result, while insurers would still be required to offer coverage to people with pre-existing conditions, insurers could charge unaffordable premiums of thousands or tens of thousands of dollars per month, effectively resulting in a coverage denial. Insurers could also offer plans with large benefit gaps. For example, before the ACA introduced the requirement that all plans cover a defined set of basic services, 75 percent of individual market plans excluded maternity coverage, 45 percent excluded substance use treatment, and 38 percent excluded mental health care, according to analysis by the Kaiser Family Foundation.[5] This would leave many people — especially those with pre-existing conditions — without access to the health services they need.
The waiver authority included in the Cassidy-Graham bill is similar to the so-called “MacArthur amendment” waivers included in the House-passed bill.[6] Analyzing those waivers, the CBO concluded that states accounting for one-sixth of the nation’s population would choose to let insurers charge higher premiums based on health status. In those states, “less healthy individuals (including those with preexisting or newly acquired medical conditions) would be unable to purchase comprehensive coverage with premiums close to those under current law and might not be able to purchase coverage at all [emphasis added].” And states accounting for half of the nation’s population would choose to let insurers exclude essential health benefits. In those states, “services or benefits likely to be excluded … include maternity care, mental health and substance abuse benefits, rehabilitative and habilitative services, and pediatric dental benefits.” People needing these services “would face increases in their out-of-pocket costs. Some people would have increases of thousands of dollars in a year.”[7]
Destabilizing Individual Market in Near Term, Risking Collapse in Long Run
Even as other members of Congress, including the chair and ranking member of the Senate Health, Education, Labor and Pensions (HELP) Committee, are working on bipartisan efforts to strengthen the individual market and the marketplaces, the Graham-Cassidy bill would disrupt the individual market in the short term. Like the Senate Republican leadership bill and the House-passed bill, it would immediately eliminate the individual mandate. That would raise the number of uninsured by 15 million relative to current law in 2018 and increase individual market premiums by 20 percent.
The bill’s elimination of the ACA marketplace subsidies and start of a block grant in 2020 would cause massive additional disruption. With 50 states and the District of Columbia left to devise their own coverage programs — lacking guidance, standards, or administrative infrastructure — and to make substantial changes to their market rules as well, insurers would have no idea how the individual market would operate starting in 2020. It could be years before they had any clarity about the state of the market, including what their risk pools would look like. In the interim, insurers would most almost certainly impose large premium rate increases to account for uncertainty; some would likely exit the market altogether.
Then in 2027, when the block grant disappeared entirely, states would no longer be able to obtain waivers of the protections for people with pre-existing conditions. Insurers in all states would face a market without an individual mandate or any funding for subsidies to purchase coverage in the individual market yet be subject to the ACA’s prohibition against denying coverage to people with pre-existing conditions or charging people higher premiums based on their health status. Many insurers would likely respond by withdrawing from the market, leaving a large share of the population living in states with no insurers, as CBO has warned about previous repeal-without-replace bills.
In both the near and long term, the disruption caused by Cassidy-Graham would thus result in large individual market coverage losses on top of those directly resulting from the bill’s marketplace subsidy cuts.
Methods Note
We estimate each state’s federal funding block grant amount in 2026 under the parameters of the Cassidy-Graham block grant formula, and compare the result to an estimate of the state’s federal funding under current law for the Affordable Care Act (ACA) Medicaid expansion to low-income adults, marketplace subsidies, and/or the Basic Health Program (BHP).
To estimate states’ Cassidy-Graham block grant amounts in 2026, we use the most recent population data for individuals with family income between 50 percent and 138 percent of the federal poverty line from the American Community Survey.
To estimate states’ federal funding under current law, we start with the Congressional Budget Office’s (CBO) March 2016 projections of national-level spending on the Medicaid expansion, marketplace subsidies, and the BHP in 2026. We apportion these amounts across the states based on the Centers for Medicare & Medicaid Services’ most recent state-level spending data for the Medicaid expansion and marketplace subsidies.
Results of our analysis reflect two limitations. First, limited data availability requires that we apportion CBO’s national-level estimate of cost-sharing reduction payments to states based on states’ premium tax credit amounts rather than cost-sharing reduction amounts. Second, CBO’s projection of Medicaid expansion spending in 2026 assumes that additional states beyond the current 31 states and the District of Columbia take up the option to expand Medicaid, but CBO does not project which specific states would do so.
Figures in Table 1 reflect the combined impact of the Cassidy-Graham block grant and the Cassidy-Graham Medicaid per capita cap. In its cost estimate for the Senate GOP leadership’s health bill, the Better Care Reconciliation Act (BCRA), CBO estimates the federal Medicaid spending cut outside of the expansion due to the per capita cap. We interpolate based on other CBO per capita cap estimates to adjust the BCRA estimate to account for both Cassidy-Graham’s changes to the per capita cap annual adjustment rate (relative to BCRA) and the plan’s exclusion of certain low-population-density states from the per capita cap through 2026. We apportion this national cut estimate in 2026 to states based on the Kaiser Family Foundation’s state-specific estimates of the federal funding impact of the BCRA per capita cap.
| TABLE 1 | |||
|---|---|---|---|
| Cassidy-Graham Block Grant and Medicaid Per Capita Cap Cut Federal Funding for Most States by 2026 | |||
| State | Estimated federal funding change, in 2026 (in $millions) | ||
| United States | -$80,000 | ||
| Alabama | 1,713 | ||
| Alaska | - 255 | ||
| Arizona | - 1,600 | ||
| Arkansas | - 1,102 | ||
| California | - 27,823 | ||
| Colorado | - 823 | ||
| Connecticut | - 2,324 | ||
| Delaware | - 724 | ||
| District of Columbia | - 431 | ||
| Florida | - 2,691 | ||
| Georgia | 1,685 | ||
| Hawaii | - 659 | ||
| Idaho | 177 | ||
| Illinois | - 1,420 | ||
| Indiana | - 425 | ||
| Iowa | - 525 | ||
| Kansas | 821 | ||
| Kentucky | - 3,062 | ||
| Louisiana | - 3,220 | ||
| Maine | - 115 | ||
| Maryland | - 2,162 | ||
| Massachusetts | - 5,089 | ||
| Michigan | - 3,041 | ||
| Minnesota | - 2,747 | ||
| Mississippi | 1,441 | ||
| Missouri | 545 | ||
| Montana | - 515 | ||
| Nebraska | 203 | ||
| Nevada | - 639 | ||
| New Hampshire | - 410 | ||
| New Jersey | - 3,904 | ||
| New Mexico | - 1,350 | ||
| New York | - 18,905 | ||
| North Carolina | - 1,099 | ||
| North Dakota | - 211 | ||
| Ohio | - 2,512 | ||
| Oklahoma | 1,118 | ||
| Oregon | - 3,641 | ||
| Pennsylvania | - 850 | ||
| Rhode Island | - 625 | ||
| South Carolina | 804 | ||
| South Dakota | 218 | ||
| Tennessee | 1,642 | ||
| Texas | 8,234 | ||
| Utah | 313 | ||
| Vermont | - 561 | ||
| Virginia | 268 | ||
| Washington | - 3,333 | ||
| West Virginia | - 554 | ||
| Wisconsin | 252 | ||
| Wyoming | -90 | ||
Source: CBPP analysis, see methods notes for details.
Cassidy-Graham’s Waiver Authority Would Gut Protections for People with Pre-Existing Conditions
Policy Basics
Health
End Notes
[1] CBPP calculations based on Congressional Budget Office estimates of July 20 version of Senate Republican leadership bill (Better Care Reconciliation Act), https://www.cbo.gov/system/files/115th-congress-2017-2018/costestimate/52941-hr1628bcra.pdf.
[2] Congressional Budget Office, “Longer-Term Effects of the Better Care Reconciliation Act of 2017 on Medicaid Spending,” June 2017, https://www.cbo.gov/system/files/115th-congress-2017-2018/reports/52859-medicaid.pdf.
[3] Edwin Park and Matt Broaddus, “Cassidy-Graham Plan’s Damaging Cuts to Health Funding Would Grow Dramatically in 2027,” Center on Budget and Policy Priorities, updated September 17, 2017, https://www.cbpp.org/research/health/cassidy-graham-plans-damaging-cuts-to-health-care-funding-would-grow-dramatically-in.
[4] Aviva Aron-Dine, “Cassidy-Graham’s Waiver Authority Would Gut Protections for People with Pre-Existing Conditions,” Center on Budget and Policy Priorities, September 15, 2017, https://www.cbpp.org/blog/cassidy-grahams-waiver-authority-would-gut-protections-for-people-with-pre-existing-conditions.
[5] Gary Claxton et al., “Would States Eliminate Key Benefits if AHCA Waivers are Enacted?” Kaiser Family Foundation, June 14, 2017, http://www.kff.org/health-reform/issue-brief/would-states-eliminate-key-benefits-if-ahca-waivers-are-enacted/.
[6] For more on the MacArthur Amendment, see Jacob Leibenluft, “MacArthur Amendment Would Mean Return to Pre-ACA Law for People with Pre-Existing Conditions,” Center on Budget and Policy Priorities, April 27, 2017, https://www.cbpp.org/blog/macarthur-amendment-would-mean-return-to-pre-aca-law-for-people-with-pre-existing-conditions.
[7] Congressional Budget Office, “H.R. 1628: American Health Care Act of 2017,” May 24, 2017, https://www.cbo.gov/system/files/115th-congress-2017-2018/costestimate/hr1628aspassed.pdf.
More from the Authors

Areas of Expertise
Recent Work: