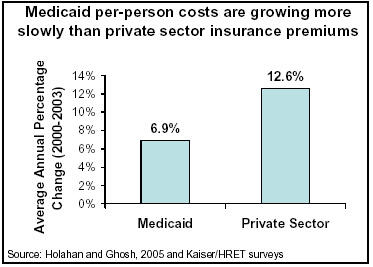
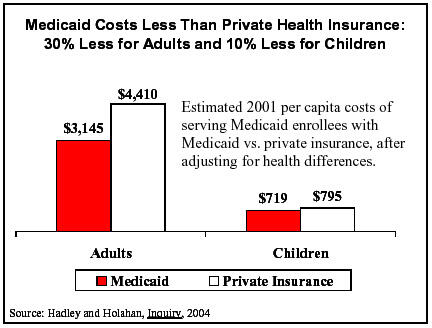
Future Medicaid Growth Is Not Due To Flaws in the Program's Design, But To Demographic Trends and General Increases in Health Care Costs
End Notes
[1] This report has also been released, in slightly altered form, as an appendix to the report, “ Cuts To Low-Income Programs May Far Exceed The Contribution Of These Programs To Deficit’s Return,” by Isaac Shapiro and Robert Greeenstein, Center on Budget and Policy Priorities, Feb. 5, 2005. Leighton Ku and Victoria Wachino also contributed to these analyses.
[2] John Holahan (director of the Urban Institute’s Health Policy Center) and Arunabh Ghosh, “Understanding the Recent Growth in Medicaid Spending, 2000-2003,” Health Affairs, January 26, 2005; Kaiser Family Foundation, news release, “A Sharp Rise in Enrollment During the Economic Downturn Triggered Medicaid Spending to Increase by One-Third from FY 2000-03,” January 26, 2005.
[3] This study also found that people with Medicaid and people with private insurance used health services at roughly comparable levels. Jack Hadley and John Holahan, “Is health care spending higher under Medicaid or private insurance?” Inquiry, 40:323-42, Winter 2003/2004. Similar findings were reached by federal researchers: see Edward Miller, Jessica Banthin, and John Moeller, “Covering the Uninsured: Estimates of the Impact on Total Health Expenditures for 2002,” Agency for Healthcare Research and Quality Working Paper No. 04407, November 2004.
[4] SCHIP stands for State Children’s Health Insurance Program; for children in low-income working families, SCHIP complements the Medicaid program.
[5] Oregon Health Research and Evaluation Collaborative, “Research Brief: Changes in Enrollment of OHP Standard Clients,” January 2004, and “Research Brief: The Impact of Program Changes in Health Care for the Oregon Health Plan Standard Population: Early Results from a Population Cohort Study,” March 2004.