- Home
- Budget Process Bill Would Result In Deep...
Budget Process Bill Would Result In Deep Cuts In Medicare and Medicaid
Summary
The Senate Budget Committee has approved a bill (S. 3521) that would radically alter federal budget procedures and could lead to deep cuts over time in the vast majority of domestic programs, including Medicaid, Medicare, and SCHIP. While the odds are slim that the legislation will be considered by the full Senate this year, the bill is nevertheless important because it appears to reflect an emerging consensus among a growing number of conservatives about how to start addressing deficits while preserving the costly tax cuts that have been enacted since 2001. Investor’s Business Daily has described this legislation — which was introduced by Senate Budget Committee Chairman Judd Gregg, has been co-sponsored by 26 other Senators (including Senate Majority Leader Bill Frist), and was approved by the Budget Committee with the support of all 12 majority party members — as a “vision statement.”[1]
The new budget procedures that the bill would establish are designed to lead to substantial reductions over time in projected spending for the vast majority of domestic programs, and to extract especially large savings from Medicare and Medicaid. As explained below, the bill’s provisions could lead to reductions in Medicare and Medicaid of unprecedented depth. A complete analysis of the legislation can be found at:
.The legislation also would force substantial reductions in appropriations for discretionary health programs, ranging from veterans’ health care to health research funded by the National Institutes of Health. The legislation would lock in, for the next three years, the overall discretionary funding levels proposed in President Bush’s most recent budget. To hit those levels, the President’s budget proposes $66 billion in domestic discretionary cuts over the next three years (relative to the 2006 funding levels for those programs, adjusted for inflation), with the cuts growing deeper each year. By 2009, the President’s proposed cuts would hit every domestic discretionary program area in the budget, except for space, science and technology. [2]
In addition, the legislation would give the President “line-item veto” authority. Although such authority is often described as a mechanism to address wasteful appropriations “earmarks” or “pork-barrel spending,” the line-item veto provisions in the Budget Committee’s bill go far beyond that. These provisions not only would give the President increased power to seek to terminate funding for entire discretionary programs, but also would grant him new authority to single out and try to cancel recently enacted provisions of law that would improve or expand entitlement programs, including Medicare and Medicaid. The President could seek to “veto” such entitlement provisions even if their cost was fully defrayed by offsetting cuts contained elsewhere in the same entitlement law.[3]
This analysis focuses, however, not on the bill’s provisions relating to discretionary programs but on the two components of the bill that would have the largest impacts on Medicare and Medicaid.
Fixed Deficit Targets Would Force Deep Cuts in Entitlement Programs, Nearly Two-thirds of Which Would Come from Medicare and Medicaid
The bill would establish a fixed deficit target for each year and would enforce those targets through automatic, across-the-board cuts in all entitlement programs other than Social Security. The automatic cuts would be triggered in any year in which the deficit target otherwise would be missed. To reach the deficit targets the bill would set for 2012 and succeeding years would require over $200 billion a year in budget cuts. [4]
- To reach the deficit target for 2012 after making the large cuts in discretionary programs that the bill envisions, entitlement cuts of unprecedented magnitude would be needed. Projected expenditures for all entitlement programs except Social Security would have to be cut by 15.6 percent (unless discretionary programs were cut even more deeply than the bill envisions, tax cuts were scaled back, or other taxes were raised).
- A reduction of 15.6 percent in Medicare would amount to a cut of $83 billon in 2012. This is the amount by which Medicare would have to be reduced if all entitlements (except Social Security) were cut by the same percentage, which is how the bill’s automatic entitlement reductions would work. Under the automatic cuts, the reductions in Medicare would likely be secured primarily (or entirely) by cutting payments to Medicare providers and Medicare plans.
- In Medicaid, a 15.6 percent reduction would translate into a federal funding cutback of $45 billion in 2012. This reduction would be achieved by cutting federal Medicaid matching payments to states by that percentage.
- The cuts in Medicare, Medicaid, and other entitlements would then grow deeper each year after 2012. By 2016, the cut in entitlement programs (other than Social Security) needed to hit the bill’s deficit target would be 17.7 percent. Over the ten years from 2007-2016, total entitlement cuts of $1.6 trillion would be needed to hit the deficit targets (unless taxes were raised or discretionary programs cut even more deeply). If all entitlement programs were reduced by the same percentage, the cumulative cuts over the ten-year period would reach $693 billion in Medicare and $360 billion in Medicaid. Cuts to these programs account for nearly two-thirds of all the entitlement cuts under the legislation. (See Figure 1)
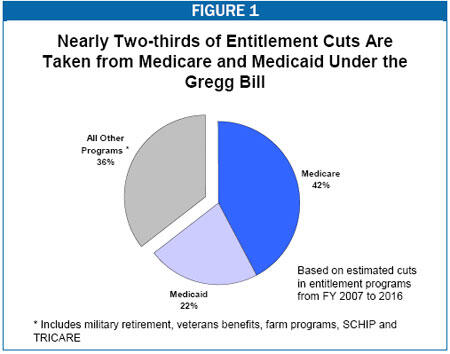
- The withdrawal of such large amounts of funding from the health-care sector not only would create serious difficulties for the over 100 million Americans who are expected to be enrolled in Medicare and Medicaid — and the hospitals, physicians, nursing homes, and pharmacies who serve them — but also would have broader effects that would be likely to ripple throughout the U.S. health care system.
Redefining Medicare and Medicaid “Solvency” to Set the Stage for Deep Program Cuts
The Senate Budget Committee bill also would establish new definitions of Medicare and Medicaid solvency and create a commission to propose measures to restore “solvency” (as so defined) to these programs, as well as to Social Security.
- In place of the definition of solvency that has applied to Medicare since its inception in 1965 —that the revenues to support the Medicare Hospital Insurance program be sufficient to meet the costs of that program — the bill would classify the entire Medicare program as being “insolvent” whenever more than 45 percent of total Medicare expenditures are financed by general revenues. To achieve this new definition of “solvency” — and to alter Medicare so that no more than 45 percent of its costs are funded by general revenues in future decades — would require Medicare cuts (or payroll tax increases) of stunning dimensions. For example, if the savings to meet this target were taken entirely out of payments to providers, those payments would have to be reduced below projected levels by 31 percent by 2030.
- >The bill also would establish a definition of solvency for the Medicaid program. Medicaid would be classified as “insolvent” in any year after 2012 in which its costs grew faster than the growth rate of the Gross Domestic Product. To satisfy the bill’s definition of Medicaid “solvency” would require cuts in projected Medicaid expenditures of 22 percent by 2020 and 50 percent by 2042.
Deficit Targets and “Solvency” Standards Would Shift Costs to States, Family Members, and Providers
These provisions of the bill would result in a “double whammy” for Medicare and Medicaid. Meeting the new “solvency” definitions would not protect Medicare and Medicaid from the automatic across-the-board cuts in entitlement programs that would be triggered when the deficit target was exceeded. The automatic cuts would be in addition to the cuts made to restore “solvency.” Conversely, even if Medicare and Medicaid were subject to very large automatic across-the-board cuts to meet the bill’s deficit targets, those cuts eventually would not be sufficient to meet the bill’s definitions of Medicare and Medicare “solvency.” Additional cuts would be needed to meet the “solvency” standards the bill would set.
These reductions in federal funding for Medicare and Medicaid would take effect at the same time that an aging baby-boom population was beginning to rely on these programs for financial protection against the rising costs of health care and long-term care. Cutting projected expenditures in Medicare and Medicaid by these large amounts would not stop the aging of the baby boomers or reduce their need for health care or long-term care. Nor would it end health-care inflation or stop the technological advances that are contributing heavily to the continued large increases in per capita health care expenditures. Cutting federal support for Medicare and Medicaid deeply would, however, force someone other than the federal government— namely, states and family members — to pick up a hefty share of the health-care costs that the federal government was shedding. It also could compel health-care providers to absorb the remaining share of those costs. And it almost certainly would lead many low-income and elderly and disabled Americans to go without various health care treatments and services they needed.
The Fixed Deficit Targets and the Automatic Entitlement Cuts
The deficit targets that the Budget Committee legislation would establish would be set at 2.75 percent of the Gross Domestic Product (the basic measure of the size of the economy) in 2007 and would shrink to 0.5 percent of GDP in 2012 and years thereafter. If the Office of Management and Budget projected that the deficit target for a year would be missed and Congress did not enact legislation producing large enough savings to hit the target, across-the-board cuts in all mandatory programs other than Social Security would be triggered automatically. The automatic cuts would be set at whatever percentage cut was needed to reach the deficit target.
Assuming that the President’s tax cuts (except for estate tax repeal) are extended and relief from the Alternative Minimum Tax is continued, the projected deficit in 2012 will exceed the bill’s target for that year by more than $200 billion even after the cuts that the bill calls for in discretionary programs are taken into account.[5] This means that unless Congress scaled back the President’s tax cuts, raised other taxes, or cut discretionary programs even more deeply than the bill calls for, $206 billion in savings from entitlement reductions would have to be produced for 2012 alone. This figure for a single year dwarfs the $39 billion in savings over five years that were contained in the Deficit Reduction Act that Congress narrowly approved earlier this year.
If Congress were unable to pass legislation achieving cuts of this magnitude, as would likely be the case, automatic entitlement cuts would be triggered. Medicare and Medicaid would be cut by $128 billion in 2012, absorbing nearly two-thirds of all the entitlement cuts under the legislation. Over the next ten years (2007-2016), a cumulative total of $1.6 trillion in entitlement cuts would be required.[6] This analysis focuses on the impact on Medicare and Medicaid.
1. Implications for Medicare
Like all entitlement programs other than Social Security, Medicare would be subject to automatic, across-the-board cuts in any year that the deficit reduction target otherwise would be missed. The Budget Committee bill imposes no limit on the percentage by which Medicare and other entitlement programs could be cut to meet the deficit targets.
Assuming that the cuts were distributed evenly across all entitlement programs — i.e., that all entitlements except Social Security were reduced by the same percentage, which is how the automatic cuts would work — Medicare would have to be cut by 15.6 percent, or $83 billion, in 2012, and by larger amounts in subsequent years.[7] This would be equivalent to reducing projected Medicare expenditures by an average of about $1,750 per beneficiary in 2012. (Note: These cuts would be in addition to the reductions in Medicare physician payment levels scheduled under current law.)
The Budget Committee bill does not specify how the automatic cuts in Medicare would be achieved. As a practical matter, automatic reductions of this magnitude probably could most readily be implemented through cuts in payments to Medicare providers, managed care plans, and drug plans.[8] The bill is silent on whether such payment reductions would have to be applied on a pro rata basis, with hospitals receiving the same 15.6 percent reduction in their reimbursements as physicians, Medicare Advantage plans, and Part D drug plans, or whether different groups of providers and plans could be subject to differing percentage reductions. If a 15.6 percent reduction were achieved through reductions in provider payments, and the reductions were applied on a pro rata basis, then:
- Medicare payments to hospitals would be cut by $28 billion in 2012;
- payments to physicians would be cut by $10 billion (in addition to the cuts scheduled under current law);
- payments to managed care plans would be cut by $14 billion; and
- payments to Part D drug plans (including subsidy payments for low-income Medicare beneficiaries) would be cut $16 billion.
The remaining cuts needed to achieve the $83 billion in reductions would come from payments to other groups of providers, such as skilled nursing facilities and home health agencies.
Reductions of this magnitude in payments to Medicare providers and plans would be unprecedented, and the effects on provider and plan behavior are unknown. It seems safe to assume, however, that the larger the Medicare patient volume, the greater the impact such reimbursement cuts would have on a provider’s or plan’s financial viability. Hospitals, physician groups, and managed care plans that are highly dependent upon Medicare revenues would have more difficulty adjusting to cuts of this magnitude than providers for whom Medicare patients constitute a small share of their operations. The adjustments that high-volume Medicare providers would be forced to make could markedly affect the accessibility and quality of the care available to their Medicare patients.
If substantial numbers of providers and managed care plans responded to the large reductions in Medicare payments by abandoning the Medicare market, the choice of providers available to Medicare beneficiaries could be restricted significantly. In addition, those providers that continued to serve Medicare patients under the reduced reimbursement rates would generally have to lower the amount and quality of care they provided to beneficiaries or to increase the prices they charged to their privately-insured patients to make up for their Medicare losses.
Similarly, some Medicare prescription drug plans likely would withdraw from the program, while those remaining in it likely would restrict more sharply the range of medications they offered, increase the amounts that beneficiaries were required to pay, and/or reduce the amounts they paid to pharmacies. The overall effect likely would be an increase in how much Medicare beneficiaries had to pay for medications and greater restrictions on the range of medications available to them through the plans.
In this environment, Medicare beneficiaries with illnesses or conditions that are very costly to treat could find themselves disfavored as patients. Another likely effect would be that private insurers and employers who had to pay higher charges to cross-subsidize providers for their Medicare losses would face greater pressure to raise their own premiums, increase patient cost-sharing, or reduce covered benefits.
2. Implications for Medicaid
Medicaid, too, would be subject to the bill’s automatic cuts. As with Medicare and other entitlements, there would be no limit on the percentage by which federal Medicaid funding could be reduced to meet the bill’s deficit targets. If the deficit targets were met through the automatic cuts (or any other approach that spread the pain evenly across entitlement programs), federal Medicaid expenditures would have to be cut 15.6 percent — or $45 billion — in 2012.
The Budget Committee legislation does not specify how the automatic cuts would be carried out in Medicaid. Unlike the Medicare program, in which federal funds flow (through fiscal agents) directly to providers and managed care plans, Medicaid is a federal-state matching program. Federal payments are made to the states, which operate the program on a day-to-day basis. The only way for the federal government to automatically achieve a specified percentage reduction in Medicaid expenditures is to reduce the payments it otherwise would make to each state by that percentage. Each state would then have to decide whether to respond to the loss of federal matching payments by reducing eligibility, increasing cost-sharing, reducing benefits, cutting payment rates for providers, or increasing its own level of funding to make up for the loss of federal funds.
Under Medicaid’s financing structure, an across-the-board reduction in federal payments to states would result in greater losses, per dollar of Medicaid expenditures, for poorer states than for affluent ones. Assume that two states each spend $200 million providing health care services for Medicaid beneficiaries during a calendar quarter and that one of these is a relatively high per capita income state — and has a 50 percent federal Medicaid matching rate — while the other state has low per capita income and a 70 percent federal Medicaid matching rate. (The matching rates vary from 50 percent to 76 percent, based on a state’s per capita income.) The 50-percent-match state would normally receive $100 million in federal matching payments for the $200 million in Medicaid costs that it incurred. Under a 15.6 percent automatic cut, this state’s federal Medicaid funding would be reduced by $15.6 million. In contrast, the poorer state would normally receive $140 million in federal matching payments for its $200 million in costs and hence would face a loss of $21.8 million in federal funds (15.6 percent of $140 million). This is a $6.2 million larger loss than the affluent state would bear.
There is no precedent for reducing federal Medicaid matching payments to states by the amounts that the bill contemplates. The $45 billion in automatic Medicaid cuts that could be triggered in 2012 alone compares to a projected reduction in federal Medicaid costs of $26.5 billion over ten years under the Deficit Reduction Act enacted earlier this year.
There also is no precedent for the types of policy changes that would have to be made to achieve savings of this magnitude. The $45 billion in federal Medicaid reductions in 2012 is equivalent to what would be saved that year by cutting payments for inpatient hospital services in half. It also is equivalent to what would be saved by eliminating about two-thirds of all payments to nursing homes for low-income seniors.
Because states have broad discretion in administering their Medicaid programs, they would differ in their responses to these reductions in federal funding. Each state would decide how to deal with the loss of federal funds, whether by cutting eligibility, increasing patient cost-sharing, limiting the scope of services, and/or reducing payments to providers and managed care plans. To the extent that states restricted eligibility, more low-income Americans would become uninsured, causing the demand for uncompensated care to rise, especially at emergency rooms.[9] To the extent that states lowered payments to providers or managed care plans, some providers and plans likely would limit their participation in Medicaid; other providers might withdraw altogether. Medicaid beneficiaries with high-cost illnesses or conditions could be placed at particular risk of losing access to providers.
Commission to Determine the “Solvency” of Medicare and Medicaid
The bill also would create a commission charged with developing a plan to ensure the long-term “solvency” of Social Security, Medicare, and Medicaid. The legislation would establish new definitions of “solvency” for Medicare and Medicaid.
The “solvency” definitions in the bill bear no relationship, however, to the actual financial status of Medicare and Medicaid. And the definitions are designed in such a way that meeting these new “solvency” standards would require deep cuts in these programs.
The commission would have 9 members appointed by Republican leaders and 6 members appointed by Democratic leaders. Ten votes would be needed to approve a commission plan. This would create a risk that the commission’s 9 Republican appointees could hang together and seek to entice a lone Democratic appointee to get to 10 votes. The plan that the commission would produce would then be moved under “fast-track procedures” in Congress with no filibusters permitted, although 60 votes would be needed to bring the legislation to a final Senate vote.
1. Implications for Medicare
Medicare would be deemed to be “insolvent,” even if the Medicare trust fund still had hundreds of billions of dollars in assets, once at least 45 percent of total Medicare costs were financed with general revenues. As a result, instead of allowing commission members to recommend ways to ensure both that Medicare remains solvent, as solvency has been understood and defined throughout the program’s history,[10] and that there is a sustainable long-term balance between overall Medicare costs and the total resources available to fund those costs, the Budget Committee legislation would compel the commission to focus on ways to ensure that no more than 45 percent of Medicare financing came from general revenues.[11]
This new definition of Medicare “solvency” has no actuarial basis, and it bears no relationship to how Medicare is funded under federal law. By law, Medicare physicians’ coverage and the new Medicare prescription drug benefit are supposed to be financed by general revenues (and beneficiary premiums), rather than by dedicated revenues (i.e., payroll taxes).
This new definition appears to be designed to achieve an ideological goal. Its restriction on general-revenue financing appears to be intended to ensure that increases in the federal income tax (such as increases from scaling back a portion of the recent tax cuts for high-income households) could not be used to address even a fraction of Medicare’s long-term financing problems, as part of a larger Medicare reform effort.
The implications for Medicare would be far-reaching. The 45-percent limitation on general-revenue financing would bar increases in general revenues to help finance the program. Increases in regressive payroll taxes would be allowed, but increases in progressive income taxes would not be.
As a consequence, if policymakers wanted to meet the 45-percent threshold without raising regressive payroll taxes, their options would be limited. They could increase beneficiary premiums and cost-sharing, with the increases growing larger each year and ultimately reaching very high levels. They could tighten Medicare eligibility rules by raising the age of eligibility or increasing the 24-month waiting period for disabled Social Security beneficiaries to qualify. They could reduce the scope of the medical services that Medicare covers. And they could freeze or cut payments to hospitals, physicians, and other Medicare providers and to Medicare managed care organizations and the new Part D drug plans. Whatever option or combination of options they chose, the cutbacks would need to grow deeper with each passing year to continue meeting the new “solvency” test.
Medicare clearly faces serious long-term financial problems. The Social Security and Medicare trustees project that the Medicare Hospital Insurance program (Medicare Part A) will become insolvent in 2019. In addition, Medicare expenditures are projected to rise rapidly in coming decades as the baby-boomers retire and health care costs continue to mount. The nation needs an honest and thoughtful debate on Medicare reform.
But the 45-percent measure would skew this debate, ensuring that progressive revenue increases are not permissible options for the commission — and ultimately Congress — to consider. Having to meet this artificial “solvency” standard would place a larger-than-necessary share of the burden of dealing with rising Medicare costs on increases in the premiums, deductibles, and co-payments that beneficiaries pay, increases in the payroll taxes that ordinary workers pay, reductions in Medicare eligibility and benefits, and reductions in the payments made to Medicare providers.
2. Implications for Medicaid
The bill also establishes a definition of Medicaid “solvency.” This is a particularly dubious undertaking; Medicaid has no trust fund or dedicated revenues, and the concept of “solvency” for a program funded by general revenues is as inapplicable to Medicaid as it would be to programs operated by the Department of Defense or the Department of Education. Nevertheless, the bill would impose a new “solvency” standard on the program, under which Medicaid would be considered insolvent in any year after 2012 in which Medicaid expenditures rose at a faster percentage rate than the Gross Domestic Product.
This definition fails to reflect the factors that are the principal drivers of Medicaid cost growth — inflation in the cost of health care services, the aging of the population, and the erosion of employer-based coverage. The bill’s so-called “solvency” definition is simply an artifice to restrict the federal government’s contribution to the Medicaid program to levels well below what is needed to keep pace with the aging of the population and rising health care costs.
The Congressional Budget Office projects, for example, that over the seven-year period from fiscal year 2007 through fiscal year 2013, the Gross Domestic Product will grow by an average of 4.9 percent per year while Medicaid costs will grow by an average of 7.8 percent annually. (These CBO estimates of Medicaid growth reflect the savings expected under the Deficit Reduction Act.)
To meet the bill’s definition of Medicaid “solvency,” the rate of growth in Medicaid spending would have to be reduced sharply. In 2013, for example, it would have to be reduced from CBO’s projected 7.7 percent growth rate for that year to 4.5 percent (the projected GDP growth rate for that year). This would translate into a reduction in federal Medicaid expenditures of $8 billion in that year, or more than twice the $4.3 billion in federal savings that the Deficit Reduction Act would achieve in 2013.
More importantly, this $8 billion would be a mere pittance compared to the vastly larger amounts by which federal Medicaid expenditures would have to be reduced in subsequent years. Limiting the growth in federal Medicaid funding to the growth rate in GDP year after year would require cuts of extraordinary depth in Medicaid over time — cuts of 22 percent by 2020, 36 percent by 2030, and 50 percent by 2042. (These cuts are relative to CBO’s estimates of Medicaid costs under current law.)
The magnitude of the Medicaid cuts that would be required to meet the bill’s “solvency” standard would be so great that the commission would likely see little alternative to proposing the abolition of Medicaid in its present form and its replacement with a block grant to states under which federal block-grant funding would rise only at the rate of GDP. Over time, that would represent a cost-shift to states of stunning dimensions — probably the largest cost-shift from the federal government to the states in U.S. history. Unless states could finance the large health-care costs that the federal government was shedding through very big state tax increases or severe cuts in other parts of state budgets such as education, they would have little alternative but to slash their state Medicaid programs deeply over time.
Shifting the Costs of Care to States, Families, and Providers
In its December 2005 analysis of the long-term budget outlook, CBO explained that “Future spending growth in [Medicare and Medicaid] will be driven by two fundamental factors: the aging of the population and growth in per-capita medical costs. The Medicare population will expand rapidly as baby boomers turn 65 and life expectancies continue to rise. Those demographic trends are also projected to increase Medicaid’s costs by boosting demand for long-term care.”[12]
CBO also pointed out in testimony before the Senate Budget Committee earlier this year that health care costs alone will continue to rise faster than GDP for the foreseeable future. CBO concluded that this reality, coupled with the projected increase in the percentage of the population over age 65, means that Medicare and Medicaid costs will necessarily rise at significant rates.[13]
Given the CBO analysis and growing concern about rising entitlement spending, the Budget Committee bill appears designed to induce deep reductions in projected Medicare and Medicaid expenditures. The bill’s deficit targets and automatic cuts in entitlement programs, and its “solvency” provisions, could lead to cuts in Medicare and Medicaid of startling proportions.
But sharply cutting federal support for Medicare and Medicaid over time will not stop the aging of the population or the accompanying increases in the need for health care and long-term care. Nor will it significantly reduce the rising costs of health care services, which are driven largely by advances in medical technology. The bill offers nothing to address the causes of growth in Medicare and Medicaid costs, other than budget-driven reductions in the federal government’s share of those costs.
Sharp Effects on Long-term Care
The large reductions in federal funding for Medicaid that would likely occur under the bill would place particular pressure on nursing home care and home and community-based services. Medicaid is the largest single purchaser of nursing home care. It is projected to finance nearly half of nursing home costs by 2015.[14]
The bill’s cuts in federal Medicaid funding would leave states with the choice of substantially increasing their own spending for long-term care services or placing the burden of making up for the loss of federal support on the backs of the families of frail elderly and disabled people who need such care. Given the magnitude of the federal cost-shift that would result under the bill, it seems likely that many states would conclude they had little choice but to shift substantial costs to beneficiaries and their families. States could seek to accomplish this by restricting eligibility for long-term care services, limiting the types of services they covered, and reducing payments to long-term-care providers while authorizing the providers to charge beneficiaries and their families substantially more.
Conclusion
CBO’s Acting Director Donald Marron recently testified that in light of the aging of the U.S. population and rapidly rising health care costs, a “substantial reduction in the growth of spending and perhaps a sizeable increase in taxes as a share of the economy will be necessary for fiscal stability to be at all likely in the coming decades.”[15] The Senate Budget Committee bill focuses exclusively, however, on cutting projected federal expenditures, while shielding tax cuts from fiscal discipline. In fact, under the bill, anything that would increase the deficit — including more tax cuts (as well as a recession, a war, or a national disaster) — would push the deficit farther above the deficit target and thereby trigger a requirement for even deeper cuts in entitlement programs such as Medicare and Medicaid.
Furthermore, while targeting Medicare and Medicaid for cuts of unprecedented depth, the bill would do nothing to address the sources of Medicare and Medicaid cost growth and the underlying problem of rapid health-care cost inflation. Through deep cuts in federal funding for Medicare and Medicaid, the bill seeks instead simply to reduce the federal government’s financial exposure for the growth in health care costs and the aging of the population. The result would be a massive shift of the costs of health care for low-income and elderly and disabled people — from the federal government to states, beneficiaries’ families, and medical care providers — and the likely loss of access to needed health care services for millions of Americans.
End Notes
[1] Jed Graham, “GOP Budget Hawks Make Push to Require Broad Spending Cuts,” Investor’s Business Daily, July 3, 2006, p. A1.
[2] The discretionary caps that the bill would establish are discussed in more detail in Arloc Sherman, James Horney, and Matt Fiedler, “Proposed Discretionary Caps Would Hit States Hard,” Center on Budget and Policy Priorities, July 5, 2006.
[3] The line-item veto legislation proposed in the bill is discussed in more detail in Richard Kogan, “Senate ‘Line-Item Veto’ Proposal Invites Abuse by Executive Branch,” Center on Budget and Policy Priorities, July 12, 2006.
[4] The bill would set the deficit target at 0.5 percent of GDP for 2012 and all succeeding years. Estimates of the entitlement cuts assume that the tax cuts, including relief from the Alternative Minimum Tax, are extended (except for the estate tax, which is assumed to be structured as provided in legislation that the House of Representatives passed on July 29, 2006). The estimates also assume that the bill’s limits on discretionary spending are adhered to through 2009 and that discretionary grows with inflation thereafter. All estimates are based on CBO’s latest projections.
[5] These deficit projections are based on the latest projections issued by CBO. In these projections, we assume that most, but not all, of the estate tax will be repealed, as prescribed under legislation approved by the House of Representatives on July 29, 2006.
[6] The need for $1.6 trillion in entitlement cuts assumes that in years after 2009, overall funding for discretionary programs would be held to the 2009 cap level that the bill would establish, adjusted only for inflation.
[7] This calculation is based on the March 2006 CBO baseline, net of Medicare premiums but not clawback payments.
[8] In theory, net Medicare expenditures could be reduced by increasing beneficiary premiums under Parts A, B, or D. In the absence of specific directions in the Budget Committee bill, however, we assume that the automatic cuts would be implemented in a way that minimizes changes in the Medicare program, i.e., by reducing payments to providers by the necessary percentage.
[9] For example, recent reports from Tennessee confirm that TennCare cutbacks instituted in that state led to substantial increases in hospital emergency room and uncompensated care costs. Todd Pack, “Charity Costs Jump Since Cutbacks in TennCare,” Tennessean, June 18, 2006.
[10] The longstanding test that the Medicare Trustees apply in determining the solvency of the program is whether the Medicare Hospital Insurance Trust Fund will have adequate assets to cover expected Medicare Hospital Insurance costs. This is the same definition of solvency used for the Social Security trust fund. In the case of Social Security, the bill does not alter the definition of solvency.
[11] For a full discussion of the issues raised by the bill’s definition of Medicare “solvency,” see Robert Greenstein, James Horney, Richard Kogan, and Edwin Park, “Senate Budget Process Legislation Embraces Misguided ‘45-Percent Trigger,’” Center on Budget and Policy Priorities, June 26, 2006.
[12] “The Long Term Budget Outlook,” Congressional Budget Office, December 2005, page 27, available at: http://www.cbo.gov/ftpdocs/69xx/doc6982/12-15-LongTermOutlook.pdf.
[13] Statement of Donald B. Marron, Acting Director, Congressional Budget Office, on “The Budget and Economic Outlook: Fiscal Years 2007 to 2016,” before the Committee on the Budget, United States Senate, Feb. 2, 2006, pages 1-2, available at: http://www.cbo.gov/ftpdocs/70xx/doc7034/02-02-OutlookTestimony.pdf.
[14] Christine Borger, et al., “Health Spending Projections Through 2015: Changes on the Horizon,” Health Affairs 25 (2006): w61-w73, published online Feb. 22, 2006, page w71.
[15] Marron, op. cit.
More from the Authors

Areas of Expertise


