Lower-Than-Expected Medicare Drug Costs Mostly Reflect Lower Enrollment and Slowing of Overall Drug Spending, Not Reliance on Private Plans
End Notes
[1] For analysis of the budget proposal to convert Medicare into a "premium support" system, see Paul N. Van de Water, "Medicare in the Ryan Budget," Center on Budget and Policy Priorities, March 28, 2012; Paul N. Van de Water, "What You Need to Know about Premium Support," Center on Budget and Policy Priorities, March 19, 2012; and Paul N. Van de Water, "Ryan-Wyden Premium Support Proposal Not What It May Seem," Center on Budget and Policy Priorities, revised December 21, 2011.
[2] See, for example, House Budget Committee Chairman Paul Ryan's March 20, 2012 address at the American Enterprise Institute, http://www.aei.org/events/2012/03/20/a-blueprint-for-american-renewal-an-address-by-house-budget-committee-chairman-paul-ryan/. See also Kathryn Nix, "Recipe for Reform: Success of Consumer-Driven Principles in Medicare Programs," Heritage Foundation, August 10, 2011 and Joseph Antos, "What Does Medicare Part D Say About the Ryan Plan?," RealClearMarkets.com, June 15, 2011.
[3] Jack Hoadley, "Medicare Part D Spending Trends: Understanding Key Drivers and the Role of Competition," Kaiser Family Foundation, May 2012.
[4] Edwin Park, "Lower-than-Expected Medicare Drug Costs Reflect Decline in Overall Drug Spending and Lower Enrollment, Not Private Plans," Center on Budget and Policy Priorities, May 5, 2011.
[5] Congressional Budget Office, "Estimates of the Effects of Medicare, Medicaid and Other Mandatory Health Provisions Included in the President's Budget Request for Fiscal Year 2013 – March 2012 Baseline," March 16, 2012.
[6] This analysis examines only the first five years of the Medicare Part D drug benefit (2006-2010) to exclude the effects of the Affordable Care Act provisions to close the so-called "doughnut hole" in the drug benefit and to charge increased premiums for higher-income beneficiaries, which began to take effect in calendar year 2011. The first of these ACA provisions increased Part D costs in 2011, while the second lowered net costs. Neither was anticipated when CBO and the Medicare actuaries issued their estimates of the drug benefit's costs when the benefit was enacted in 2003.
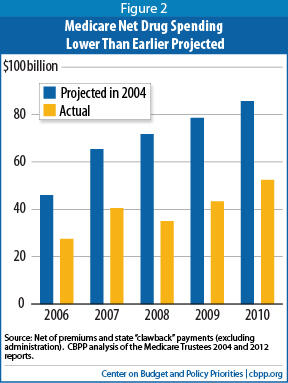
[7] CBPP analysis of 2004 and 2012 Medicare Trustees' Reports. These figures exclude administrative costs (and are net of premiums and "clawback" payments through which states continue to contribute a share of the cost of providing drug coverage to dual eligible beneficiaries).
[8] CBPP analysis of Congressional Budget Office, "Letter to the Honorable Don Nickles," November 20, 2003, Congressional Budget Office, "Letter to the Honorable Joe Barton," February 16, 2005; and CBO Medicare baselines.
[9] For purposes of this analysis, Part D enrollment also includes individuals who receive employer-sponsored retiree drug coverage subsidized by Medicare Part D.
[10] The Medicare trustees only report actual enrollment and projected enrollment by calendar year. These figures reflect an adjustment to estimate enrollment by fiscal year.
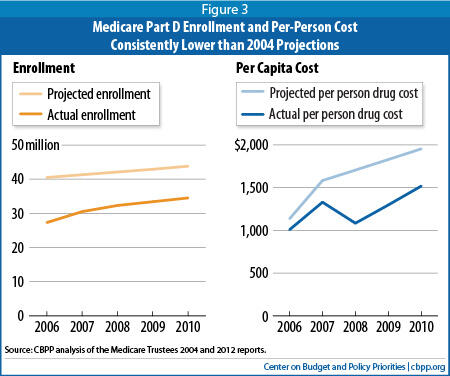
[11] CBO did not project specific year-by-year enrollment figures but had assumed that on average, about 93 percent of Medicare Part B beneficiaries would enroll in the Medicare drug benefit (or receive employer-sponsored retiree drug coverage subsidized by Medicare) during its first eight years.
[12] In 2010, actual costs were $1,519 per beneficiary compared to projected costs of $1,955 per beneficiary, according to the Medicare trustees. These per-beneficiary cost figures exclude administration and are net of premiums and state clawback payments.
[13] In 2010, according to CBO estimates, actual costs were $1,532 per beneficiary compared to projected costs of $1,824 per beneficiary.
[14] See Mark Merlis, "Explaining the Growth in Prescription Drug Spending: A Review of Recent Studies," U.S. Department of Health and Human Services, August 2000.
[15] See, for example, Aaron Catlin et al., "National Health Spending in 2006: A Year of Change in Prescription Drugs," Health Affairs, January/February 2008; Micah Hartman et al., "National Health Spending in 2007: Slower Drug Spending Contributes to Lower Rate of Overall Growth Since 1998," Health Affairs, January/February 2009; Micah Hartman et al., "Health Spending Growth at a Historical Low," Health Affairs, January 2010; Anne Martin et al., "Recession Contributes to Slowest Annual Rate of Increase in Health Care Spending in Five Decade," Health Affairs, January 2011; Hoadley, op cit; and IMS Institute for Healthcare Informatics, "The Use of Medicines in the United States: Review of 2010," April 2011.
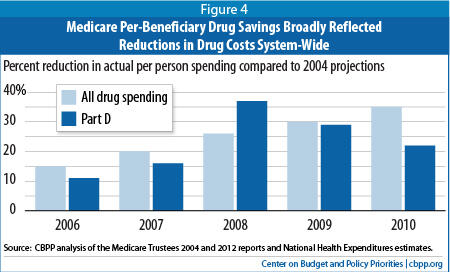
[16] CBPP analysis of National Health Expenditure projections and data.
[17] See, for example, the 2007-2010 Medicare Trustees' reports and Hoadley, op cit.
[18] Murray Aitken and Ernst Berndt, "Medicare Part D at Age Five: What Has Happened to Seniors' Prescription Drug Prices?," IMS Institute for Healthcare Informatics, July 2011.
[19] Antos, op cit.
[20] HHS Office of Inspector General, "Generic Drug Utilization in the Medicare Part D Drug Program," November 2007.
[21] James Capretta, "The Top Five Flawed Arguments Against Premium Support," Heritage Foundation, January 30, 2012.
[22] Hoadley, op cit.
[23] 2008 is the exception as Medicare Part D per beneficiary costs fell between 2007 and 2008, in large part because insurers repaid Medicare for overpayments they received in 2006. (Insurers had overestimated their expected costs in their plan bids for 2006.) In addition, according to the Medicare trustees, premium receipts were higher than expected in 2008.
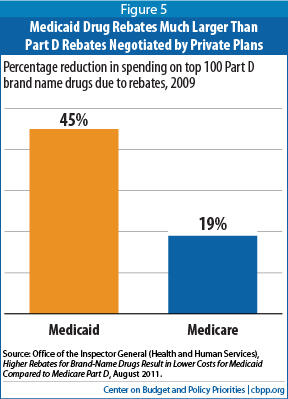
[24] Under a "best price" provision, drug manufacturers must provide state Medicaid programs the same level of rebates that they provide most other public and private purchasers if the rebates that they provide to other purchasers exceed certain minimum amounts. As part of the Medicare drug law, Congress specifically excluded Medicare Part D rebates from the calculation of best price because of concerns that the best price provision could interfere with the expected ability of private plans to negotiate larger rebates than those required under Medicaid.
[25] The gap between Medicaid and Medicare rebates is likely larger today because the Affordable Care Act increased Medicaid drug rebates starting in 2010. See HHS Office of Inspector General, "Higher Rebates for Brand-Name Drugs Result in Lower Costs for Medicaid Compared to Medicare Part D," August 2011. See also Richard Frank and Joseph Newhouse, "Mending the Medicare Prescription Drug Benefit: Improving Consumer Choices and Restructuring Purchasing," The Hamilton Project at the Brookings Institution, April 2007; Stephen Schondelmeyer, Statement before the Minority Office of the House Committee on Government Reform, January 2006; and House Committee on Oversight and Government Reform, "Medicare Part D: Drug Pricing and Manufacturer Windfalls," July 2008, http://oversight.house.gov/documents/20080724101850.pdf.
[26] Congressional Budget Office, "Estimates of the Effects of Medicare, Medicaid and Other Mandatory Health Provisions Included in the President's Budget Request for Fiscal Year 2013 – March 2012 Baseline," March 16, 2012.
[27] Hoadley, op cit.